Resident Goals, Preferences, & Priorities (GPP) - What Matters to Me
The Moving Forward Coalition is leading a national effort to strengthen person-centered care by developing and scaling a practical approach to elevating each individual’s Goals, Preferences, and Priorities (GPP) in both care planning and day‑to‑day life.
Why GPP Matters
Older adults and people with disabilities who live in nursing homes thrive when their goals, preferences, and priorities shape their care. Strengthening pathways for each person’s input enhances dignity, experience of care, and relationships among residents, staff, and care partners/family members. This work builds on the Coalition’s 2023–2024 Residents’ Goals, Preferences, and Priorities Action Plan, developed through national engagement with residents, care partners, staff, researchers, operators, and advocates. The Action Plan identifies the need for consistent, meaningful processes to ask older adults about What Matters to them, document and communicate goals, preferences, and priorities with nursing home team members, and scale and spread a consistent approach across U.S. nursing homes.
Why Action is Needed Now
One of the top ten federal nursing home deficiency citations most years is for F-tag 656: Comprehensive Care Plans. In many cases, this may reflect a failure to individualize person-directed care plans with each older adult. Nursing home staff may lack standardized, easy-to-use tools to ask older adults about their goals, preferences, and priorities, document that information, and share each older person’s stated goals with relevant team members. In addition, processes vary widely across nursing homes, and documentation systems are not always designed to capture What Matters most to residents. This inconsistency may limit person-centered care and increases the risk that nursing home surveyors may cite a deficiency related to care planning.
These gaps underscore the need for a shared, practical approach based on consensus from residents, care partners/family members, direct care staff, and system leaders to promote person‑centered principles guiding care planning and everyday practice.
From Consensus to Guide
How national engagement shaped the GPP Guide
Over the past two decades, many nursing homes have made important efforts to strengthen person‑centered care and improve how they gather residents’ goals, preferences, and priorities (GPPs). Yet, we know that GPP processes still vary widely: from who is asked, to how information is captured, where it is documented, and whether it is reliably integrated into day‑to‑day care.
In direct response to the National Academies of Sciences, Engineering, and Medicine (NASEM) Nursing Home Report recommendation to strengthen person‑centered assessment and care planning, the Coalition convened a committee dedicated to person-centered care. This group brought together residents, care partners/family members, direct care staff, clinicians, advocates, and subject‑matter experts to align on a consensus‑based action plan for improving how nursing homes identify, document, and implement residents’ goals, preferences, and priorities in their care plans and daily care. Through this collaborative process, the group reviewed and discussed shared principles and lived experience and co-designed a practical guide to support more consistent, resident‑centered GPP implementation across diverse nursing home settings.
With this Guide and Process, Nursing Home Teams can:
Apply an evidence-based model that builds on—and strengthens—existing person‑centered care practices.
Identify, document, and deliver care that reflects each older adult’s goals, preferences, and priorities.
Create opportunities for improving care, support, and culture in alignment with What Matters most to residents.
From Guide to Practice
How nursing homes are implementing the Guide with structured support
The GPP Guide centers care planning around the resident, with input from staff, care partners, and others through structured conversations and simple, practical workflows that make What Matters most visible and actionable in daily care. Practice-based experience is generating ongoing lessons for strengthening person-centered care that will be integrated into future versions of the Guide and process.
Kansas State University currently leads implementation, providing hands-on coaching and learning support to help nursing homes embed GPP practice recommendations into care planning and daily practice.
2024-2025 Pilot Cohorts: Six nursing homes in Kansas partnered with KSU to pilot the GPP guide and process, testing implementation in real‑world settings.
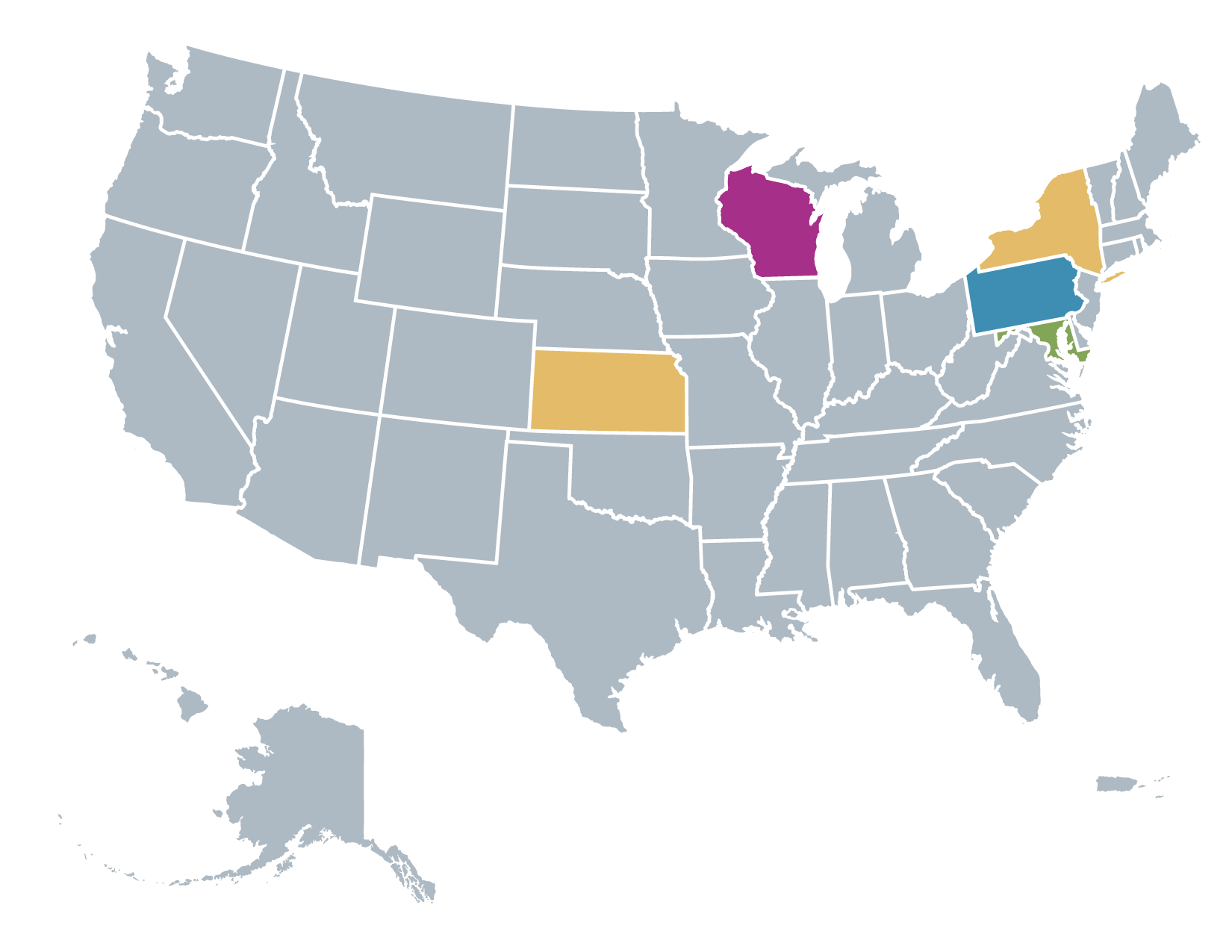
Expanded Implementation: Building on early lessons, the pilot has expanded to 22 nursing homes across Kansas, Wisconsin, New York, Pennsylvania, and Maryland, through a combination of in‑person and virtual learning cohorts designed to support scale and sustainability.
Thank you to our partner: Kansas State University.
From Practice to Continuous Learning
How practice-based experience is generating lessons for strengthening person-centered care
Early findings suggest that structured GPP processes support stronger engagement and clearer care practices. Residents and families report feeling more respected and included in decisions that affect daily life. Staff report increased confidence in providing individualized care. Nursing homes are learning how more consistent, accessible documentation of resident priorities can support both person‑centered care and compliance with federal care planning requirements.
From Learning to Policy
How implementation insights inform system‑level change
What we learn from GPP implementation will shape national policy recommendations, including opportunities to improve surveyor guidance, strengthen staff training expectations, and better align person-centered care practices with federal quality measures.
GPP Repository
How implementation insights inform system‑level change
What we learn from GPP implementation will shape national policy recommendations, including opportunities to improve surveyor guidance, strengthen staff training expectations, and better align person-centered care practices with federal quality measures.


Note: The GPP Guide specifically focuses on processes addressing a resident’s GPPs only and is not intended to address the entire care planning process.
The Moving Forward Coalition is continuing to learn how to further enhance the Guide with input from nursing home staff. If you would like to share feedback, please click here.